Medical and physician associate (PA) programs have increased clinical exposure by expanding standardized patient encounters, investing in simulation, and redesigning clerkships.
But more exposure has not produced more consistent preparation. In one survey, nearly 68% of physician associate educators report deficiencies in students' differential diagnosis proficiency. In another survey of U.S. internal medicine clerkship directors, 84% of students were rated as having poor (29%) or fair (55%) clinical reasoning when entering the clerkship.
Despite rotating across different sites, services, and preceptors — and participating in simulations, OSCEs, and standardized patient encounters — learners often lack consistent assessment of their clinical reasoning because of what patients they encounter. This variability makes readiness difficult to assess and costly to address. AI-enabled simulation brings assessment earlier and standardizes how learners are evaluated, cutting down on late-stage remediation and manual review.
Why does uneven clinical exposure create uneven assessment?
Clinical exposure has increased across training programs, yet insight into learner readiness remains inconsistent. With varying exposure to clinical scenarios and levels of diagnostic complexity, differences in student performance reflect opportunity rather than comparable experience.

What uneven exposure looks like in practice
- Learners in the same cohort encounter very different chief complaints, acuity levels, and diagnostic complexity
- Some learners regularly engage in diagnostic uncertainty, hypothesis generation, and refinement
- Others have limited opportunities to practice reasoning because cases are stable, protocol-driven, or predictable
Why this creates an insight gap
- Performance differences often reflect opportunity, not ability
- Faculty cannot reliably compare learners who have faced different clinical demands
- Reasoning gaps stay hidden until core rotations, when remediation is harder and more resource-intensive
Why can't traditional evaluations overcome exposure variability?
Medical and PA programs have long relied on exams, OSCEs, SP encounters, and preceptor evaluations to assess readiness. While each method plays an important role, they do not consistently surface clinical reasoning. In one survey, only 42.7% of students reported that preceptor evaluations gave them insight into their clinical reasoning, reflecting the limits of episodic, context-dependent assessment rather than the quality of instruction itself.
Tool limitations
- Written assignments: measure knowledge, not reasoning processes
- OSCEs: assess communication and structured tasks, but often capture outcomes rather than diagnostic pathways
- SPs: high fidelity but expensive (upwards of $900 per student) and capacity-limited, with variable feedback quality
- Simulations: expensive and access-limited, making diagnostic reasoning difficult to observe consistently
Evaluator variability
- Assessments depend heavily on evaluator background and training. One study finds that 36% of Pediatric Critical Care Medicine faculty had not participated in any formal teaching skill development as faculty.
- Preceptor evaluations are shaped by local case mix and individual interpretation
- Narrative feedback is time-intensive, uneven, and often delayed
How does AI simulation standardize clinical reasoning assessment?
Simulation itself is not new in medical and PA education. What is new is the ability to use AI-driven simulation as a standardized, scalable assessment of clinical reasoning — not just an isolated learning activity.
AI simulation-based assessment addresses the core problem of uneven exposure by creating a controlled environment where every learner encounters comparable diagnostic complexity and decision-making demands. Rather than relying on chance clinical encounters, programs can intentionally design when and how reasoning is observed.
What AI simulation makes possible
- Standardized, clinician-developed case exposure ensuring every learner engages with comparable diagnostic complexity regardless of rotation site or patient mix
- Consistent AI-enabled evaluation of clinical reasoning driven by clear scoring criteria, structured prompts, and rubric application aligned to competencies and milestones
- Early, comparable insight into readiness that surfaces reasoning gaps before learners enter high-stakes clinical environments
- OSCE-equivalent simulation at up to 80% lower cost enabling scale without proportional increases in staffing or scheduling complexity
- Reduced faculty burden by using AI to capture reasoning steps and generate structured assessment data without additional faculty review time
With DDx
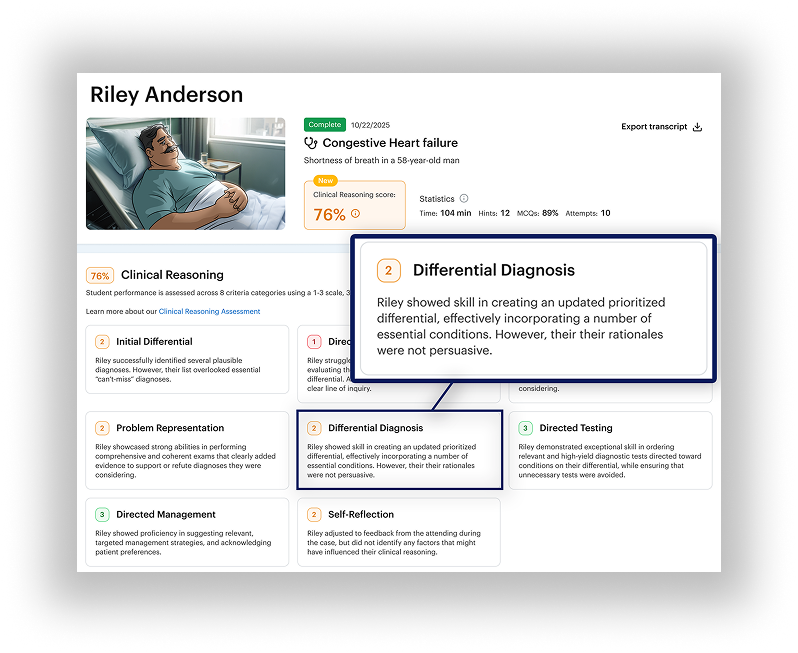
DDx is designed to bring consistency to clinical reasoning assessment while accommodating the distinct goals of medical and PA education. By standardizing the cognitive demands learners encounter rather than the patients they happen to see, DDx allows programs to evaluate clinical reasoning fairly and comparably without constraining how or where learners train. Every learner reasons through comparable diagnostic complexity and uncertainty regardless of rotation site, clinical reasoning is evaluated at the level of judgment and decision-making rather than exposure alone, and readiness insight reflects shared cognitive demands rather than chance clinical encounters.
Frequently asked questions
How does DDx reduce faculty workload while improving clinical reasoning assessment?
DDx automates case delivery, student feedback, and performance tracking — eliminating the manual review work that typically accompanies OSCE and SP-based assessments. Faculty time shifts from scoring and logistics to interpreting cohort-level analytics and targeting instruction. The result is more actionable data with less total faculty effort per student assessed.
At what point in training should programs introduce standardized clinical reasoning assessment?
The earlier the better. Programs that introduce standardized simulation in pre-clinical or early clinical training establish a baseline before exposure variability compounds, identify individual and cohort-level patterns when remediation is still low-stakes, and build longitudinal evidence of reasoning development that supports milestone reviews and accreditation documentation.
